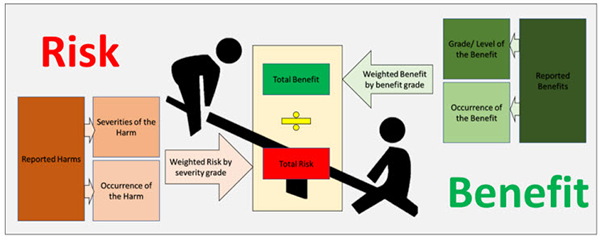
Benefits and Risks
In the expansive terrain where science meets hope, families of children with Duchenne Muscular Dystrophy find themselves facing a landscape both promising and perilous. The clinical trial—that singular path between laboratory discovery and approved treatment—stretches before them like an unmarked trail across difficult country.
Here, the landmarks of methodical research rise against horizons of urgent need, creating a geography where calculation and emotion, evidence and faith, must somehow find their balance. Parents stand at this crossroads carrying the weight of impossible decisions: whether to venture into the unknown territory of experimental treatments or remain on the more certain but limited path of established care.
The journey through DMD clinical trials demands a particular kind of courage—one that acknowledges risks while refusing to surrender to the merciless progression of the disease. It is a journey that transforms not only individual lives but also reshapes our collective understanding of what treatment might someday mean for this condition that has, for too long, claimed childhoods with impunity.
Potential Benefits of Clinical Trial Participation
Access to Novel Treatments Participation in clinical trials offers families affected by DMD the opportunity to access cutting-edge therapies years before they might become commercially available. Given the progressive nature of DMD, this early access could mean preservation of muscle function during critical developmental windows that would otherwise be lost to the natural disease course. For example, a child enrolled in an exon-skipping trial at age 6 might maintain walking ability into adolescence when they might otherwise have lost mobility by age 10-12.
Comprehensive Medical Monitoring Clinical trial protocols typically include more frequent and comprehensive monitoring than standard care.
Participants often receive:
- Regular cardiac evaluations with advanced imaging
- Detailed pulmonary function testing
- Sophisticated muscle function assessments
- Careful monitoring of bone health and other potential complications
- Access to specialists who might otherwise have long waiting periods
This intensive monitoring can identify complications earlier than routine care might, potentially leading to earlier interventions for issues like cardiac involvement or declining respiratory function.
Contribution to Scientific Knowledge Families often derive significant meaning from knowing their participation advances understanding of DMD, potentially helping thousands of children in the future. This altruistic motivation can provide purpose and agency in the face of a condition that often leaves families feeling powerless. The data collected—even from trials that don’t meet their primary endpoints—contributes to the refined understanding of DMD progression and treatment response.
Financial Considerations While not a primary reason for participation, many trials cover costs associated with:
- Study medications and procedures
- Travel expenses to research centers
- Lodging during study visits
- Medical evaluations that might otherwise be partially covered or denied by insurance
This reduction in financial burden can be significant for families already facing substantial medical and adaptive equipment expenses.
Community and Support Participation connects families with others navigating similar experiences, creating valuable support networks. The research teams involved in DMD trials often include professionals with deep expertise who can provide guidance beyond the study protocol itself. This sense of connection and access to knowledge can reduce the isolation many DMD families experience.
Significant Risks and Challenges
Unknown Safety Profiles
Experimental treatments carry inherent uncertainties about both short and long-term safety:
- Novel gene therapies may trigger immune responses with unpredictable consequences
- Antisense oligonucleotides may have off-target effects on other genes
- Systemic effects may impact organs beyond targeted muscles
- Long-term safety data is inevitably limited during trials
In the DMD community, safety concerns have materialized in several high-profile cases, including unexpected cardiac events in gene therapy trials and serious adverse events leading to clinical holds.
Physical and Emotional Burden The logistics of trial participation can be demanding:
- Frequent travel to specialized research centers, often requiring significant time away from school and work
- Invasive procedures including muscle biopsies, blood draws, and sometimes lumbar punctures
- Demanding testing protocols that can be physically exhausting for children with limited strength
- Emotional roller-coaster of hope and disappointment as interim results emerge
These burdens fall on children already navigating the physical and emotional challenges of a progressive disability.
Placebo Assignment Risk
Many trials include placebo control groups, meaning some participants will not receive the experimental treatment during the controlled phase:
- For a progressive condition like DMD, time spent on placebo represents irreversible disease progression
- The psychological impact of possibly receiving placebo can be significant
- Even with eventual crossover designs, the delay in receiving active treatment may mean missing critical windows for functional preservation
- This reality creates profound ethical tension between rigorous trial design and individual patient benefit.
Opportunity Costs Participation in one trial typically excludes simultaneous enrollment in others:
- Families must make difficult choices between promising approaches
- Exclusion criteria often bar participants from future trials for certain periods
- The commitment to one experimental path may close doors to others that subsequently show greater promise
This forced selection creates a significant decision burden at a time when robust comparative data is unavailable.
Therapeutic Misconception
Many families enter trials with expectations exceeding the likely outcomes:
- Even in later-phase trials, individual responses vary substantially
- Early-phase trials primarily assess safety, not efficacy
- The primary purpose remains research, not guaranteed treatment
- This gap between hope and reality can lead to profound disappointment when trials don’t meet personal expectations.
Special Considerations in DMD Clinical Trials
Age and Disease Stage Factors The heterogeneous nature of DMD progression creates complex inclusion criteria:
- Younger children may have more preservation potential but less ability to complete demanding assessments
- Older participants may be more motivated but have less reversible disease
- The “plateau phase” in mid-childhood can complicate detection of treatment effects
- Window of opportunity for certain interventions may be narrow and tied to specific functional stages
These factors mean that promising treatments may show effects in some populations but not others, creating challenging risk-benefit calculations for individual families.
Genetic Mutation Specificity
Many DMD therapies target specific genetic mutations:
- Exon-skipping approaches only work for certain deletion patterns
- Gene therapy approaches may have differing effects based on underlying mutations
- Pre-existing antibodies to viral vectors may exclude some participants from gene therapy trials
- Ultra-rare mutations may have limited trial opportunities
This genetic stratification creates inequities in access to promising research.
Decision-Making Complexities Families must navigate particularly complex informed consent issues:
- Children with DMD may have cognitive involvement affecting comprehension
- Parental decision-making occurs under extreme emotional stress
- Risk tolerance differs substantially between families
- Decision fatigue compounds over years of managing the condition
Medical information is highly technical and evolving rapidly
Healthcare providers and researchers must carefully balance providing realistic information without eliminating hope that drives participation.
Balancing the Scales
For families considering clinical trial participation, the decision requires weighing several factors:
- The child’s current trajectory and functional status
- The specific mechanism and preliminary evidence for the experimental treatment
- The family’s capacity to manage trial logistics and demands
- Alternative options currently available or on the horizon
- The child’s own wishes and tolerance for procedures
- The potential impact on quality of life during the trial period
Ideally, this complex decision-making occurs with support from:
- Neuromuscular specialists familiar with both standard care and research landscape
- Genetic counselors who can explain mutation-specific implications
- Patient advocacy organizations providing peer perspective
- Ethics consultation when conflicts or complexities arise
- Mental health professionals supporting the emotional dimensions
The path through clinical trials in DMD exemplifies medicine at its most hopeful and most uncertain—where the quest for transformative treatments meets the reality of methodical science and the urgency of childhood development. For families navigating this terrain, each decision represents a profound act of both courage and love.
American Psychological Association. (2020). Publication manual of the American Psychological Association (7th ed.). https://doi.org/10.1037/0000165-000

